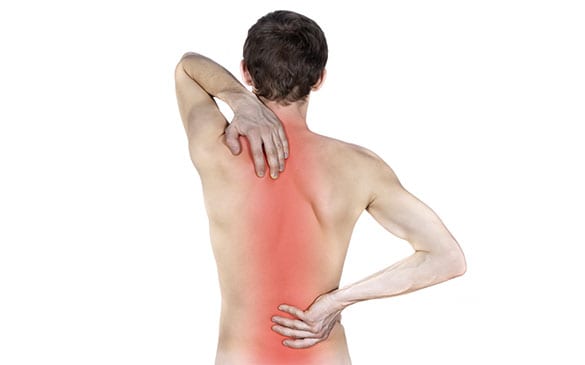
Learn more about Herniated Discs and how LA Orthopedic Group can help.
The 33 bones in the five major regions of the spine are cushioned by spongy discs. The purpose of these discs is to minimize friction and allow the backbone and its joints to carry out daily movements. If one of these discs becomes damaged, soft, jelly-like material on the inside may press through a crack in the harder exterior covering.
- A herniated disc can cause little or no pain
- Pain is experienced due to compression on a nerve root
- Most patients respond well to conservative treatments
CONTACT US TODAY
Signs of a Herniated Disc
Nerve irritation often results in pain felt somewhere along the nerve’s pathway (radicular pain), but not always at the point where there is nerve compression. For instance, pressure on the sciatic nerve coming from the lower spine and extending to parts of the legs may be felt in the hips, buttocks, thighs, or legs. The most common location of disc herniation is in the lower back. Possible symptoms include:
- Pain associated with certain movements
- Weakness in legs or arms
- Numbness and general weakness
- “Pins and needles” sensations or tingling
- Neck pain extending to shoulders and arms
- Lower back pain extending to lower extremities
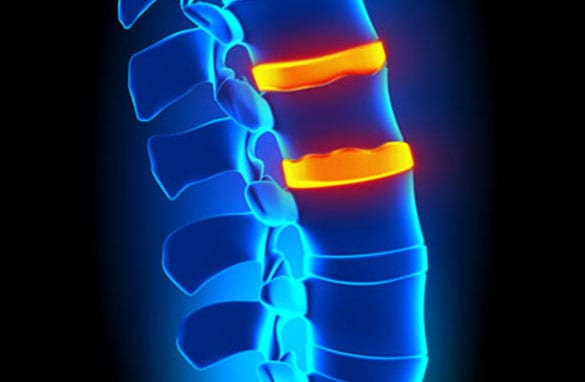
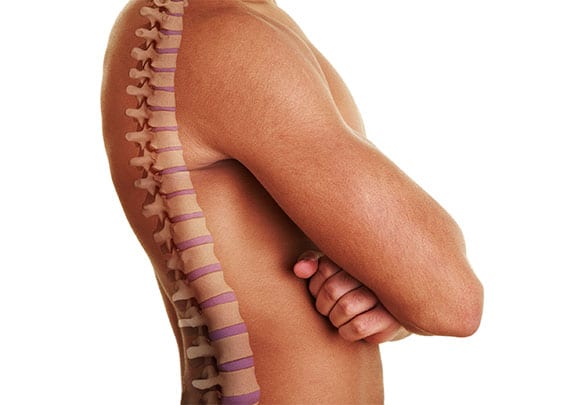
Why Discs Become Herniated
Spinal discs may become damaged due to normal age-related wear. Other age-related conditions like arthritis and osteoporosis sometimes contribute to fractures in vertebrae or facet joints (joints of the spine) that may cause a disc to slip out of place and irritate nerves. Discs may also become herniated from an injury affecting the spine. Contributing factors include weight, genetics, and occupation, especially work that involves heavy lifting or repetitious back-related movements.
Diagnosing Herniated Discs
Image tests pinpoint the exact location of the damage disc. MRI and CT scans provide greater detail than X-rays alone. Diagnosis could also include a myelogram (injection of dye into spinal fluid), nerve testing, and the use of epidural injections or nerve blocks to confirm that the suspected nerve that’s causing the pain is the one affected.
Possible Treatments
Physical therapy that includes heat and cold applications, a patient-specific exercise routine, and massage therapy and the use of anti-inflammatory and pain medications and spinal decompression therapy are among the initial attempts often made to treat a herniated disc. Avoiding certain movements that trigger pain can also provide relief.
Surgical Options
If the herniated disc is a confirmed source of a patient’s pain and other treatments aren’t effective, surgery may be recommended. Common procedures include microdiscectomy to remove the damaged part of the disc. Fusion surgery may be necessary if removal of part or all of the disc causes the spine to become unstable.
The best way to decrease your odds of having a herniated disc is to keep your spine and its supporting muscles, discs, and tissues as healthy as possible. It’s a goal often achieved by getting regular exercise, avoiding excessively sugary and fatty foods, drinking plenty of water, and paying attention to your posture. If you do experience pain that may be from a damaged disc, an orthopedic specialist may be able to recommend treatment options you haven’t yet considered.